The possible causes of pericarditis or pericarditis are as diverse as the respective treatment options. Prevention is difficult when the chances of recovery are usually good.
What is pericarditis?
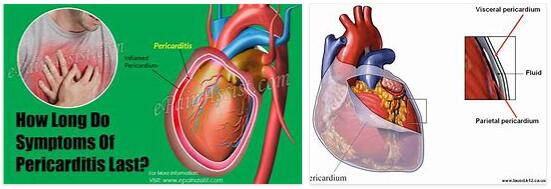
According to abbreviationfinder.org, the pericardium is a sheath of tissue that surrounds the heart. This tissue covering is also known as the pericardium. In medicine, the inflammation of the pericardium is therefore also referred to as pericarditis.
Cardiac inflammation is symptomatically noticeable in those affected, for example by severe pain below the breastbone. This pain often worsens with physical activity or deep breathing. In addition to the pain, pericarditis can also lead to fever.
A distinction can be made between what is known as primary pericarditis and secondary pericarditis. The more common primary and the less common secondary pericarditis differ, among other things, in their underlying causes.
Cardiac inflammation can be accompanied in many cases by a so-called pericardial effusion (i.e. a pericardial effusion). This causes fluid to accumulate in the pericardium.
Causes
There are various causes that can underlie pericarditis. While primary pericarditis is caused by viruses in most cases (in rarer cases also by bacteria), diseases that do not primarily affect the heart are responsible for secondary pericarditis.
If no clear cause can be assigned to pericarditis, this is also referred to in medicine as idiopathic pericarditis.
Viral pericarditis is often caused by so-called Coxsackie viruses. But influenza viruses or adenoviruses can also be responsible for pericarditis.
Bacteria that cause pericarditis often originate from sites of inflammation in the body and are transported to the heart via the blood. Finally, secondary pericarditis can be caused, for example, by various cancers in which metastases form in the pericardium.
Symptoms, Ailments & Signs
Acute pericarditis most often presents with pain in the chest and behind the breastbone, often radiating to the left arm, neck, or back, and may be aggravated by coughing, breathing, swallowing, or changing body position. Symptoms can sometimes improve if people sit up straight and bend their upper body forward. Fever is also possible.
Other symptoms can include increased heart rate and cardiac arrhythmias. If the course is severe, chest tightness and shortness of breath can also occur. Since similar symptoms can also be signs of a heart attack or pneumonia or pleurisy, a doctor should be consulted immediately and the cause clarified.
In the case of chronic pericarditis, it is possible that there are no or hardly any symptoms or that they develop so slowly that they are overlooked for a long time. Those affected initially only feel a general exhaustion and only as the disease progresses do symptoms such as an accelerated heartbeat, congestion in the neck veins, initially symptoms during physical exertion, later also at rest and the formation of edema develop.
Diagnosis & History
In order to diagnose pericarditis, the treating doctor usually first asks the patient about his or her medical history and performs a physical examination with a stethoscope.
If pericarditis is suspected, an ECG can be performed and blood can be taken (the latter to obtain indications of inflammation).
In most cases, pericarditis takes a good healing process. Especially if the pericarditis is caused by viruses, healing often occurs after just a few weeks. In some cases, however, complications can arise if, for example, the pericarditis spreads to other structures of the heart.
Another complication is cardiac tamponade. The pressure of the pericardium on the atria becomes so high that the blood pressure drops sharply.
Complications
With the right treatment, acute pericarditis usually heals without complications. However, if pericarditis is left untreated, life-threatening heart problems can develop. First, there is a risk that the inflammation will spread to other layers of the heart and lead to inflammation of the heart muscle or the inner lining of the heart. Cardiac tamponade can also occur.
Fluid accumulates in the pericardium and presses on the heart, which in extreme cases can lead to cardiogenic shock. In the long term, such a pericardial effusion can cause other diseases and symptoms such as bleeding or right- sided heart failure. Chronic inflammation of the pericardium can lead to a so-called “armoured heart”, in which the pericardium hardens and calcifies like a capsule.
In the long term, an armored heart can lead to permanent heart damage and severely impair the heart’s pumping function. In addition, permanent congestion-related kidney or liver damage can occur, which is associated with further complications.
A swollen liver can lead to swelling of the legs and accumulation of fluid in the abdominal cavity. A damaged kidney can cause high blood pressure, poisoning and other problems. In addition, those affected are usually very exhausted and suffer from various accompanying symptoms.
When should you go to the doctor?
In any case, one should consult a doctor immediately if physical symptoms such as pain on the left side of the chest and behind the breastbone occur during an infection, especially if you feel weak at the same time.
Especially with bacterial infections or in people with autoimmune diseases there is an increased susceptibility to pericarditis. But even if there is no infection, symptoms that can indicate heart problems should always be taken seriously and in any case should be clarified by a doctor.
Anyone who is quickly exhausted, has a repeated tendency to fever and often suffers from heart pain should seek medical treatment immediately, because untreated heart disease can be life-threatening. The earlier treatment begins, the better the chances of recovery.
If pain behind the breastbone and shortness of breath occur with a flu-like infection with fever and the circulatory system is so unstable that there is a risk of circulatory collapse, an emergency doctor must be called immediately. In addition, in the event of shortness of breath and a suspected heart attack, first aid must be provided until the emergency doctor and ambulance arrive.
Treatment & Therapy
For a successful therapy of pericarditis, the diagnosis of the corresponding causes is important, among other things, in order to be able to treat any underlying diseases. Regardless of the cause, in the case of pericarditis, physical rest through bed rest is usually necessary first. While in many cases the pericarditis can be treated with medication, in some cases an operation is necessary.
If a pericarditis is caused by viruses, there are options for drug therapy, including the administration of anti-inflammatory and pain-relieving drugs. Here it is primarily possible to combat the symptoms. If bacteria are behind a pericarditis, they can also be combated with antibiotics.
If, for example, secondary pericarditis is based on an autoimmune disease, therapy can integrate immunosuppressive drugs. If kidney failure is responsible for the inflammation of the pericardium, dialysis may be necessary in addition to drug treatment.
If, for example, cardiac tamponade occurs as part of a pericarditis, a possible surgical measure, the so-called pericardial puncture, is necessary. The fluid that is pressing on the ventricles of the heart is drained from the pericardium. If the fluid builds up quickly, it may also be necessary to place a cardiac catheter during the procedure to continuously drain the fluid from the pericardium.
Outlook & Forecast
Pericarditis can result in the premature death of those affected without medical care. The inflammation can spread further in the organism to the surrounding areas and lead to a steady deterioration in health. The functional activity of the heart is thus significantly restricted and can lead to irregularities and failures.
In the event of an unfavorable course, there is a risk of an acute health condition that can trigger lifelong health impairments or lead to the death of the person concerned. In an acute condition, an operation is often necessary to stabilize the patient. Subsequently, rehabilitation measures and restructuring of lifestyle habits must be carried out, since the general performance of the person concerned is reduced.
With early and good treatment, the prognosis is good. Thanks to the medical care and good therapy options, the pericarditis heals completely in most patients. If no complications occur, the patient can usually be discharged from treatment after a few weeks as symptom-free.
In drug therapy, the pathogens are prevented from spreading and killed at the same time. The stronger and healthier the patient’s body’s defense system is, the faster healing is possible. If there are other illnesses or if cardiac activity is impaired overall, recovery may be delayed. Nevertheless, a cure is possible.
Prevention
There are few ways to prevent pericarditis. If a patient is affected by repeated inflammation of the pericardium, for which no cause can be assigned, the administration of a prophylactic medication is occasionally possible in consultation with the attending physician.
Aftercare
The cause of the inflammation of the pericardium (pericarditis) is decisive for the treatment and thus also for the follow-up care. In the case of viral pericarditis, the painkillers and anti-inflammatory drugs prescribed by the doctor should be taken in the recommended amount and duration. If another underlying disease is the cause of the pericarditis, then its treatment is also necessary.
With chronic pericarditis, it is important to be aware of the symptoms so that you can act quickly when the first signs appear. In addition, a regular cardiological examination should be carried out. In principle, it is advisable to prevent infections in all forms of pericarditis.
General hygiene measures, vaccinations if necessary and avoidance of other risks of infection should always be considered here. It is particularly important to refrain from any physical exertion or sporting activity during the healing process.
Sport and heavy physical work should only be taken up slowly after the pericarditis has completely subsided and, if necessary, stopped again if the symptoms recur.
Other activities that put a heavy strain on the heart, such as greasy food, smoking and a generally unhealthy lifestyle, should be recognized as risk factors and stopped if possible. Regular cardiac examinations should be performed.
You can do that yourself
People who have been diagnosed with pericarditis can support medical treatment with a number of measures and various household and natural resources.
Bed rest is particularly important, because recovery is optional and without complications only if you take it easy. Those affected should also eat healthily, avoid stress and ensure regular but moderate physical activity. Drug therapy can be supported by natural means. In addition to herbal tea made from chamomile or lemon balm, gentle preparations made from valerian are also available.
In the case of severe pain in the heart area, however, the doctor should be consulted. In general, medical supervision is necessary for pericarditis, especially in the case of previous illnesses and other risk factors.
However, certain home remedies such as warm wraps or pads can be used in most cases. After consultation with the doctor, various homeopathic remedies can be tried. For example, the remedy Kali carbonicum or “potash” has proven itself. Asclepias tuberosa or Kalmia help with sharp chest pains. If the pericarditis does not go away despite all measures, a further medical examination is necessary.